Part
One: Characteristics and Causes of Trigeminal Neuralgia
III.
Types of Trigeminal Neuralgia and Their Causes
A. Introduction
We define seven forms of TN: typical
TN, atypical TN, pre-TN,
multiple-sclerosis-related TN, secondary
TN, post-traumatic TN (trigeminal neuropathy),
and failed TN. These forms of TN should
be distinguished from idiopathic (atypical)
facial pain, as well as other disorders
causing cranio-facial pain.
B.
Typical Trigeminal Neuralgia (Tic Douloureux)
 This
is the most common form of TN, that has previously been termed Classical,
Idiopathic and Essential TN. Nearly all cases of typical TN are caused
by blood vessels compressing the trigeminal nerve root
as it enters the brain stem. This neurovascular or microvascular compression
at the trigeminal nerve root entry zone may be caused by arteries of veins,
large or small, that may simply contact or indent the trigeminal nerve. In people
without TN, blood vessels are usually not in contact with the trigeminal nerve
root entry zone.
This
is the most common form of TN, that has previously been termed Classical,
Idiopathic and Essential TN. Nearly all cases of typical TN are caused
by blood vessels compressing the trigeminal nerve root
as it enters the brain stem. This neurovascular or microvascular compression
at the trigeminal nerve root entry zone may be caused by arteries of veins,
large or small, that may simply contact or indent the trigeminal nerve. In people
without TN, blood vessels are usually not in contact with the trigeminal nerve
root entry zone.
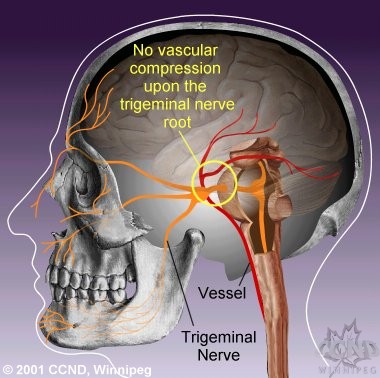
| In
people without TN, there is usually no vascular compression upon the trigeminal
nerve root. |
|
|
| |
 |
|
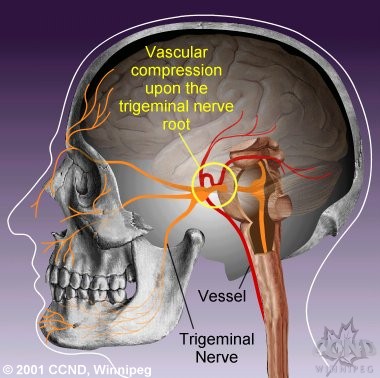
In
most sufferers of typical trigeminal neuralgia, vessels compress the trigeminal
nerve root. |
|
|
|
|
|
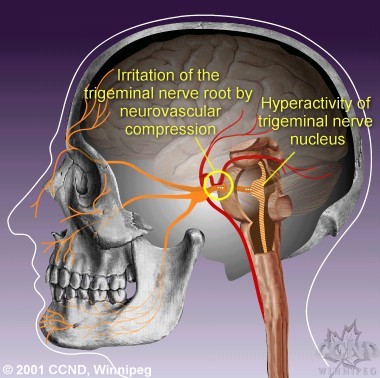
Pulsation of vessels upon the trigeminal nerve
root do not visibly damage the nerve. However, irritation from repeated pulsations
may lead to changes of nerve function, and delivery of abnormal signals to the
trigeminal nerve nucleus. Over time, this is thought to cause hyperactivity
of the trigeminal nerve nucleus, resulting in the generation of TN pain.
 |
The generation
of TN pain is thought to result from peripheral pathology (i.e. neurovascular
compression) and central pathophysiology (i.e. hyperactivity of the trigeminal
nerve nucleus). |
The superior cerebellar artery is the vessel most
often responsible for neurovascular compression upon the trigeminal nerve root,
although other arteries or veins may be the culprit vessels. TN may be cured
by an operation that effectively relieves the neurovascular compression upon
the trigeminal nerve root. This operation is called microvascular
decompression, and is described in Part
Two: Treatment of Trigeminal Neuralgia.
C. Atypical
Trigeminal Neuralgia
 Atypical TN is characterized by a unilateral,
prominent constant and severe aching, boring or burning pain superimposed upon
otherwise typical TN symptoms. This should be differentiated from cases of typical
TN that develop a minor aching or burning pain within the affected distribution
of the trigeminal nerve.
Atypical TN is characterized by a unilateral,
prominent constant and severe aching, boring or burning pain superimposed upon
otherwise typical TN symptoms. This should be differentiated from cases of typical
TN that develop a minor aching or burning pain within the affected distribution
of the trigeminal nerve.
Vascular compression, as described above in typical
TN, is thought to be the cause of many cases of atypical TN. Some believe atypical
TN is due to vascular compression upon a specific part of the trigeminal
nerve (the portio minor), while others theorize that atypical TN
represents a more severe form or progression of typical TN.
Atypical
TN pain can be at least partially relieved with medications
used for typical TN, such as carbamazepine
(Tegretol®). MVD surgery is curative for many patients with atypical
TN, but not as reliably as for those with typical TN. It is also important to
note that rhizotomy procedures may be effective
in treating atypical TN, but are more likely to be complicated by annoying or
even painful numbness (i.e. deafferentation pain).
D.
Pre-Trigeminal Neuralgia
Days
to years before the first attack of TN pain, some sufferers experience odd sensations
in the trigeminal distributions destined to become affected by TN. These odd
sensations of pain, (such as a toothache) or discomfort (like "pins and
needles", parasthesia), may be symptoms of pre-trigeminal neuralgia. Pre-TN
is most effectively treated with medical therapy
used for typical TN. When the first attack
of true TN occurs, it is very distinct from pre-TN symptoms.
E.
Multiple Sclerosis-Related Trigeminal Neuralgia
The
symptoms and characteristics of multiple sclerosis (MS)-related TN are identical
to those for typical TN. Two to four percent
of patients with TN have evidence of multiple sclerosis and about 1% of patients
suffering from multiple sclerosis develop TN. Those with MS-related TN tend
to be younger when they experience their first attack of pain, and the pain
progresses over a shorter amount of time than in those with typical TN. Furthermore,
bilateral TN is more commonly seen in people with multiple sclerosis.
MS involves the formation of demyelinating plaques within the
brain. When these areas of injury involve the trigeminal
nerve system, TN may develop. MS-related TN is treated with the same medications
used for typical TN (see Medications). Trigeminal
rhizotomies are employed when medications fail
to control the pain. For some individuals with MS and TN, neurovascular compression
of the trigeminal nerve root may be a rare cause and demonstrated with special
MRI or CT scans. In such cases, microvascular decompression
surgery may be considered for treating the MS-related TN.
F.
Secondary or Tumor Related Trigeminal Neuralgia
Trigeminal
neuralgia pain caused by a lesion, such as a tumor, is referred to as secondary
trigeminal neuralgia. A tumor that severely compresses or distorts the trigeminal
nerve may cause facial numbness, weakness of chewing muscles, and/or constant
aching pain (also see Trigeminal Neuropathy
or Post-Traumatic Trigeminal Neuralgia). Medications
usually help control secondary TN pain when first tried, although often become.
Surgically removing the tumor usually alleviates pain and trigeminal function
may return. At the time of surgery, after the removal of the tumor, the trigeminal
nerve may be found to also be compressed by an artery or vein that causes the
typical features of TN. This vessel must then be moved away from the nerve by
microvascular decompression techniques to cure TN.
|
|
|
 |
| |
|
|
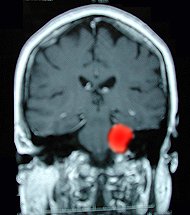
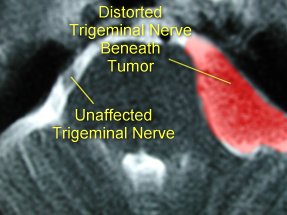
In these
MRI images, a tumor responsible for compressing the trigeminal nerve
is highlighted in red.
|
G. Trigeminal
Neuropathy or Post-Traumatic Trigeminal Neuralgia
Injury
to the trigeminal nerve may cause this severe pain
condition. Trigeminal Neuropathy or Post-Traumatic TN may develop following
cranio-facial trauma (such as from a car accident), dental trauma, sinus trauma
(such as following Caldwell Luc procedures) but most commonly following destructive
procedures (rhizotomies) used for treatment of
TN. Following TN injury, numbness may become associated with bothersome sensations
or pain, sometimes called phantom
pain or deafferentation pain. These pain conditions are caused by
irreparable damage to the trigeminal nerve and secondary hyperactivity of the
trigeminal nerve nucleus.
The
pain of trigeminal neuropathy or post-traumatic TN is usually constant, aching
or burning, but may be worsened by exposure to triggers such as wind and cold.
Such deafferentation pain can start immediately or days to years following injury
to the trigeminal nerve. In the most extreme form, called anesthesia
dolorosa, there is continuous severe pain in areas of complete numbness.
Unfortunately,
treatment of post-traumatic TN is often ineffective and pain
may not be controlled with medications. There
are some reports of pain relief associated with the use of trigeminal nerve
stimulation procedures. More invasive procedures such as brain surface (pre-motor
cortex) stimulation, or focused injuries in the brain stem (tractotomy) have
also been tried.
H.
"Failed" Trigeminal Neuralgia
Not
all cases of TN may be effectively controlled with any one form of medications
or surgical interventions. When medications
are no longer effective, surgical interventions are
considered. If pain recurs or persists following surgery, medications are tried
again and may then work more effectively. Rarely, additional or repeated surgical
interventions are necessary. Unfortunately, in a very small proportion of sufferers,
all medications, microvascular
decompression and destructive rhizotomy procedures
prove ineffective in controlling TN pain. This condition is called "failed"
trigeminal neuralgia. Such individuals also often suffer from additional trigeminal
neuropathy or post-traumatic TN as a result of the destructive interventions
they underwent. Investigational treatments may be considered including stimulation
of the brain surface (pre-motor cortex stimulation), controlled lesioning of
the brain stem (tractotomy), or stimulation of the trigeminal nerve or Gasserion
ganglion (trigeminal nerve stimulation).
Prepared by A.
M. Kaufmann & M.
Patel
© 2001 Centre for Cranial Nerve Disorders, Winnipeg, University of Manitoba,
Health Sciences Centre. The information provided on this web-site is intended
for educational purposes only, and should not be used to diagnose or treat a disease
or disorder. This information is not intended to substitute, supplement, or in
any way qualify the services or advice provided by a qualified health care professional.
Please consult with a certified health care professional before pursuing any form
of medical action. Duplication in any part or form of this document is strictly
prohibited. All rights reserved. For further information please read our disclaimer.
Web-Site related inquiries can be directed to the Information
Provider.
 This
is the most common form of TN, that has previously been termed Classical,
Idiopathic and Essential TN. Nearly all cases of typical TN are caused
by blood vessels compressing the trigeminal nerve root
as it enters the brain stem. This neurovascular or microvascular compression
at the trigeminal nerve root entry zone may be caused by arteries of veins,
large or small, that may simply contact or indent the trigeminal nerve. In people
without TN, blood vessels are usually not in contact with the trigeminal nerve
root entry zone.
This
is the most common form of TN, that has previously been termed Classical,
Idiopathic and Essential TN. Nearly all cases of typical TN are caused
by blood vessels compressing the trigeminal nerve root
as it enters the brain stem. This neurovascular or microvascular compression
at the trigeminal nerve root entry zone may be caused by arteries of veins,
large or small, that may simply contact or indent the trigeminal nerve. In people
without TN, blood vessels are usually not in contact with the trigeminal nerve
root entry zone. 


 Atypical TN is characterized by a unilateral,
prominent constant and severe aching, boring or burning pain superimposed upon
otherwise typical TN symptoms. This should be differentiated from cases of
Atypical TN is characterized by a unilateral,
prominent constant and severe aching, boring or burning pain superimposed upon
otherwise typical TN symptoms. This should be differentiated from cases of